Dr. Sudeshna Saha
Hysteroscopic Surgeon in Kolkata, West Bengal, India
For Appointment Call + 91 98302 45993
Call Between Monday to Saturday 8 A.M. TO 6 P.M.
WhatsApp
+91 98302 45993


For Appointment Call + 91 98302 45993
Call Between Monday to Saturday 8 A.M. TO 6 P.M.
WhatsApp
+91 98302 45993


Hysteroscopy Procedure
A number of different sizes and types of hysteroscope are available. The choice of instrument varies according to the purpose of the procedure and whether surgical procedures are to be performed at the same time.
Sometimes, hysteroscopy using narrow-diameter hysteroscopes can be performed without anesthesia. Local anesthetic can also be applied topically or given by injection. In some cases, dilation of the cervical opening with medications known as prostaglandins and/or surgical instruments may be necessary. A vaginal speculum is often inserted prior to the procedure to facilitate insertion of the hysteroscope through the cervical os (opening). After insertion of the hysteroscope, fluid or gas is injected into the uterine cavity to distend the uterus and thus improve visualization.
Some mild cramping may be experienced during the procedure, depending upon the type of anesthesia used. If necessary, short-acting analgesics or sedatives medications may be given intravenously if necessary.
Hysteroscopy Risks and Complications
Complications of hysteroscopy are rare. The most common complication that has been reported is accidental perforation of the uterus. Other possible (but rare) complications include bleeding, infection, damage to the urinary or digestive tract, and medical complications resulting from reactions to drugs or anesthetic agents. Other rare complications are fluid overload or gas embolism (when gas bubbles enter the bloodstream) from the liquid or gas that is injected to distend the uterine cavity during the procedure.
Hysteroscopy Follow-up
It is important for the woman to adhere to the doctor's recommendations regarding follow-up examinations and visits. Inform your physician if you are experiencing any adverse effects or recurrence of symptoms.
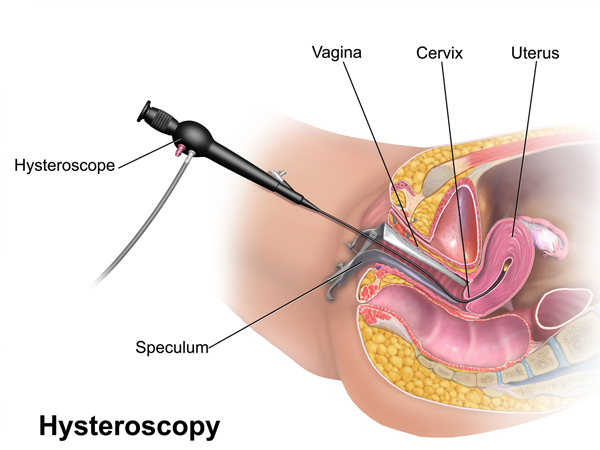
What is a hysteroscopy for?
Hysteroscopy is a diagnostic and surgical procedure that makes examining the inside of the uterus possible without making an abdominal cut (incision). During hysteroscopy, a lighted viewing instrument called a hysteroscope is inserted through the vagina and cervix and into the uterus.
What is a hysteroscopy for?
Hysteroscopy is a diagnostic and surgical procedure that makes examining the inside of the uterus possible without making an abdominal cut (incision).
During hysteroscopy, a lighted viewing instrument called a hysteroscope is inserted through the vagina and cervix and into the uterus.
What is hysteroscopy and endometrial biopsy?
Hysteroscopy is the exam of the inside of the cervix and uterus using a thin, lighted, flexible tube called a hysteroscope. Your healthcare provider inserts the device through the vagina. Your provider may use hysteroscopy to: Take a tissue sample (biopsy) Remove polyps or fibroid tumors.
How do they remove polyps from uterus
The removal of endometrial or cervical polyps is a relatively simple procedure. Some cervical polyps are completely seen outside the cervix and can be removed in a doctor's office or surgery with an instrument called a polyp forceps. Endometrial polyps and deeply inserted cervical polyps require a hysteroscopy.
What happens during a hysteroscopy
A hysteroscopy is a simple procedure usually carried out on an outpatient or day-case basis. This means you won't normally need to stay in hospital overnight.
Preparing for a Hysteroscopy
In the days and weeks before a hysteroscopy, you may be advised to:
have tests to check whether you can have the procedure, such as blood tests and a pregnancy test - these may be done at an appointment about a week before your hysteroscopy use contraception - a hysteroscopy can't be carried out if you're pregnant.
stop smoking - if you're due to have a general anaesthetic and you smoke, stopping smoking in the lead up to the procedure can help reduce your risk of complications from the anaesthetic
If you're going to have fibroids removed, you may be given medicine to help shrink them beforehand.

On the day of your Hysteroscopy
If you're having a general anaesthetic, you'll need to avoid eating or drinking for a few hours before the procedure. Your appointment letter will mention whether this applies to you.
If you're having no anaesthetic or just a local anaesthetic, you can eat and drink as normal.
It's a good idea to wear loose, comfortable clothes when you arrive for your appointment, as you'll be asked to remove any clothes from below your waist and change into a hospital gown for the procedure.
You can bring a friend or relative with you for support, although they may not be allowed in the room during your hysteroscopy.
The Hysteroscopy Procedure
A hysteroscopy usually takes between 5 and 30 minutes. During the procedure:
you lie on a couch with your legs held in supports and a sheet is used to cover your lower half
an instrument called a speculum may be inserted into your vagina to hold it open (the same instrument used for a cervical screening test), although this isn't always needed.
the vagina and cervix are cleaned with an antiseptic solution
a hysteroscope (long, thin tube containing a light and camera) is passed into your womb - you may experience some cramping and discomfort as it passes through your cervix
fluid is gently pumped into the womb to make it easier for your doctor to see inside
the camera sends pictures to a monitor, so your doctor or specialist nurse can spot any abnormalities.
In some cases, a small sample of tissue from the womb lining may be removed for further testing. This is known as an endometrial biopsy.
If you're having a hysteroscopy to treat a condition such as fibroids or polyps, fine surgical instruments can be passed along the hysteroscope. These are used to cut or burn away the abnormal tissue.
What happens after a hysteroscopy
You should be able to go home on the same day as your hysteroscopy. If you had an anaesthetic, you may need to stay in hospital for a few hours until it has worn off.
You can drive yourself home if no anaesthetic or only local anaestheticwas used. If you had a general anaesthetic, you won't be able to drive for at least 24 hours, so you'll have to arrange for someone to take you home.
Recovering at home
It's a good idea to rest when you get home. If you had a general anaesthetic, someone should stay with you for at least 24 hours until the effects of the anaesthetic have worn off. Don't drive or drink alcohol during this time.
While you recover, you may experience:
Cramping that's similar to period pain - this should pass in a few days and you can take regular painkillers such as paracetamol or ibuprofen in the meantime
Spotting or bleeding - this can last up to a week or more; use sanitary towels rather than tampons until your next period to help reduce the risk of your womb or cervix (entrance to the womb) becoming infected
These side effects are normal and nothing to worry about, but you should seek medical advice if they are particularly severe.
Returning to your Normal Activities
Most women feel they can return to normal activities, including work, the day after having a hysteroscopy. Some women return to work later the same day.
However, you may wish to have a few days off to rest, particularly if you had treatment such as fibroids removal and/or a general anaesthetic was used.
Your doctor or surgeon can advise you about any activities you need to avoid while you recover, but generally speaking:
You can eat and drink as normal straight away - if you feel a bit sick after a general anaesthetic, try eating small, light meals at first
You can have a shower the same day or the next day
You should avoid having sex for a week, or until any bleeding stops - this will help to reduce the risk of infection